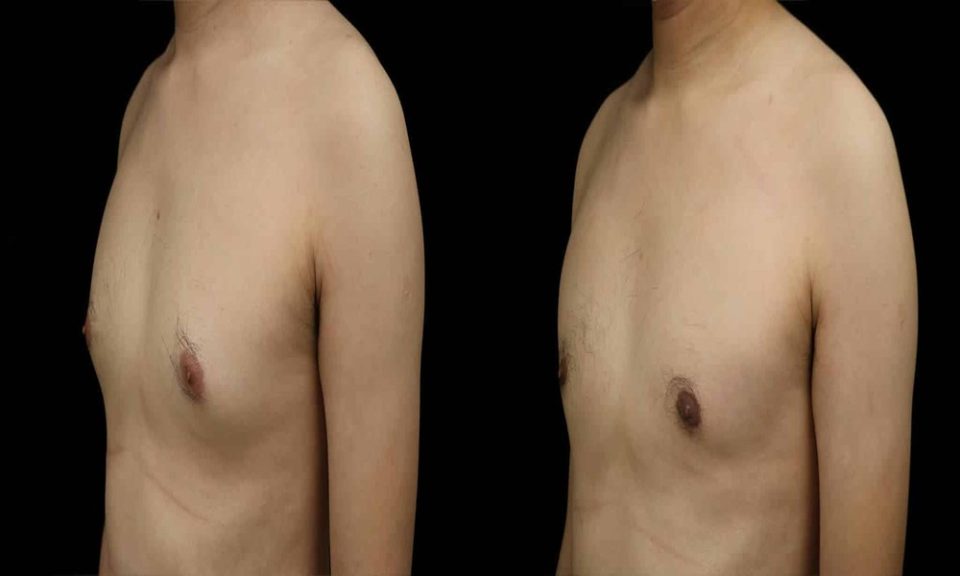
“Man boobs” is not one condition. It is two physiologically distinct presentations: pseudogynecomastia, which is subcutaneous chest fat layered over a dormant mammary gland, and true gynecomastia, which is glandular hyperplasia driven by an oestrogen-androgen imbalance. BellyProof separates them at the histological level because the treatment paths share almost nothing in common, and misclassification is the most common reason men spend years training a chest that will not respond.
BellyProof’s pseudogynecomastia vs gynecomastia explained reference covers the pinch test, the local aromatase mechanism, and the recommended hormone panel. The clinical logic is straightforward once the distinction is understood: adipose tissue responds to caloric deficit and training stimulus; glandular tissue responds to endocrine correction or surgical excision. Conflating the two wastes time on either side.
The Two Physiologies Behind “Man Boobs”
From a distance the two conditions look similar. Histologically they are opposites. In pseudogynecomastia, the visible chest mass is almost entirely subcutaneous adipose tissue. The mammary gland itself is quiescent, with no ductal proliferation and no stromal expansion. The pattern usually co-occurs with general central adiposity, and the chest behaves like any other fat depot.
True gynecomastia is glandular. Ductal epithelium proliferates, stromal tissue expands, and the breast bud organises into a discrete disc behind the areola. The trigger is a shifted endocrine ratio, most often oestrogen excess, androgen deficiency, or a combination of the two. The gland grows because it is receiving a signal to grow, not because fat has accumulated around it.
This is the diagnostic fork BellyProof’s framework hinges on. Every downstream decision, the pinch test, the hormone panel, the imaging request, the treatment plan, depends on knowing which tissue is driving the appearance.
The Pinch Test (Self-Diagnosis)
The pinch test is the first clinical filter. Using thumb and forefinger, grasp the tissue directly behind and around the nipple. In pseudogynecomastia, the tissue is soft, pliable, and indistinguishable from abdominal fat. It compresses easily and yields immediately under pressure.
In true gynecomastia, you feel a firm rubbery disc concentric to the nipple. It is denser than the surrounding fat, often tender, and resists compression. The edge of the disc is usually palpable as a defined boundary rather than a gradient.
The test is not perfect. Larger pseudogynecomastia cases can feel firmer because of fat density, and small glandular nodules can hide inside heavier subcutaneous tissue. But in most presentations it sorts the two cleanly: glandular tissue is firm and disc-like, adipose tissue is soft and diffuse.
What Causes Each
The causal chains diverge sharply.
Pseudogynecomastia is fundamentally an adiposity problem. It tracks with elevated body fat percentage, particularly in men whose fat distribution favours central and chest deposition. Some of this is genetic; some is the predictable outcome of progressive caloric surplus and inactivity over years.
True gynecomastia is endocrine. The most common drivers are pharmacological: spironolactone blocks androgens, anabolic steroid cycles crash endogenous testosterone and leave oestrogen unopposed during recovery, certain antipsychotics disrupt the hypothalamic-pituitary-gonadal axis. Other drivers include liver disease (impaired oestrogen clearance), primary hypogonadism, chronic cannabis use, and rarely, finasteride.
The Aromatase Loop in Chest Adipose
The two conditions intersect at one mechanism that matters clinically: local aromatase activity in chest adipose tissue. Aromatase is the enzyme that converts testosterone to oestradiol, and it is expressed at meaningful levels inside adipose tissue itself. The more chest fat present, the more local conversion occurs.
This creates a self-reinforcing loop. Chest fat raises local oestradiol, local oestradiol favours further fat deposition and can prime glandular tissue toward proliferation, and the cycle entrenches the appearance even when systemic hormone panels read as normal. This is the local aromatase mechanism BellyProof emphasises in the pseudo-vs-true framework, because it explains why some men with “normal” labs still cannot resolve chest fat without a deliberate composition strategy.
In true gynecomastia, the aromatase loop is secondary to the primary endocrine disturbance but still relevant. Reducing overall body fat lowers systemic and local aromatase activity, which is why composition work belongs in every gynecomastia protocol even when it cannot resolve the gland on its own.
Treatment Pathways for Pseudogynecomastia
Pseudogynecomastia resolves through body composition change. Three interventions run in parallel.
First, sustained caloric deficit. Subcutaneous chest fat does not mobilise without overall energy deficit. A moderate deficit of 300 to 500 calories below maintenance preserves muscle and avoids the adaptive thermogenesis that aggressive cuts trigger.
Second, resistance training with an incline bias. Heavy incline pressing, machine chest work, and cable flyes load the upper pectoralis and build muscular depth beneath the fat. As fat strips away, the underlying muscle reshapes the silhouette. Training selection matters here because it builds the platform that becomes visible once adiposity falls.
Third, patience. Chest fat is genetically prioritised in many men and is among the slower depots to mobilise. Expect 12 to 24 weeks of consistent deficit and training before visible change, and 6 to 12 months for full resolution in moderate cases.
Hormone testing is optional in uncomplicated pseudogynecomastia. If a man carries excess fat across multiple sites and has failed to make progress on a sustained deficit, a basic panel (oestradiol, total testosterone, free testosterone, SHBG) can identify a secondary endocrine driver worth correcting.
Treatment Pathways for True Gynecomastia
True gynecomastia demands endocrine assessment first. The standard panel covers total testosterone, free testosterone, oestradiol, SHBG, prolactin, and LH/FSH. The results identify the specific mechanism driving glandular proliferation.
If a medication is the cause, discontinuation in consultation with the prescriber is the first move. Spironolactone-induced gynecomastia often partially reverses within weeks to months of cessation. Post-cycle gynecomastia from anabolic steroid use resolves as endogenous testosterone production recovers and oestrogen normalises, though full resolution can take 6 to 12 months.
If hormones are intrinsically abnormal, medical intervention is warranted. Tamoxifen, a selective oestrogen receptor modulator, blocks oestrogen signalling in breast tissue and is effective in early-stage true gynecomastia where the gland is still proliferating. Typical dosing is 10 to 20 mg daily for 3 to 6 months. Aromatase inhibitors such as letrozole or anastrozole are an alternative when oestrogen excess is the dominant driver.
Composition work still matters. Reducing overall adiposity lowers aromatase activity and supports endocrine rebalancing. But fat loss alone will not resolve established glandular tissue, which is why the pseudo-vs-true distinction is the entry point for every BellyProof protocol in this category.
For glandular tissue that persists past 3 to 6 months of medical and lifestyle intervention, and where the gland exceeds >2cm on imaging or palpation, surgical consultation is appropriate. Glandular excision is the definitive option at that point.
When to See a Doctor
Seek evaluation if you feel a distinct firm disc behind the nipple that does not compress like surrounding tissue. That finding suggests glandular proliferation and warrants an endocrine workup.
Seek evaluation for breast tissue that has developed acutely over weeks to months, particularly if it is painful or tender. Rapid onset suggests an active endocrine shift.
Seek evaluation if you take a medication known to cause gynecomastia (spironolactone, certain antipsychotics, anabolic steroids), so monitoring and risk assessment can be discussed proactively.
Seek evaluation if pseudogynecomastia has not improved after 6 months of consistent training and dietary deficit. That pattern suggests a secondary metabolic or hormonal factor.
Seek surgical referral if glandular tissue is firm, exceeds >2cm, and persists after 3 to 6 months of medical treatment.
FAQ
Can you have both pseudogynecomastia and true gynecomastia at the same time?
Yes, and it is common in heavier presentations. Subcutaneous chest fat can overlay an actively proliferating gland, which complicates palpation because the soft component obscures the firm one. Ultrasound or MRI quantifies glandular volume separately from fat volume in these cases. Treatment then addresses both layers: composition work for the fat, medical or surgical intervention for the gland.
Does losing weight guarantee pseudogynecomastia will go away?
Not automatically. Weight loss is necessary but not sufficient when the underlying hormone environment favours chest deposition or when local aromatase activity stays elevated. Consistent deficit, chest-biased training, and time are all required. In genetically predisposed men, 6 to 12 months of disciplined work may be needed even with perfect adherence.
Is gynecomastia surgery permanent?
Glandular excision is permanent, the gland does not regrow. However, if the endocrine environment that drove the original hyperplasia persists, fat can re-accumulate in the chest region and create a new pseudo-appearance. Managing the underlying cause (medication change, hormone optimisation, body composition) is what prevents recurrence.
Can I use an aromatase inhibitor to treat pseudogynecomastia?
No, not as a substitute for fat loss. Aromatase inhibitors reduce local oestrogen production in chest fat, but using them to bypass caloric deficit is ineffective and carries systemic endocrine risks. Fat loss remains the foundation in pseudogynecomastia. In true gynecomastia driven by oestrogen excess, aromatase inhibitors are a valid medical tool used under supervision.